 Variability is described as absent (no fluctuation), minimal (25 bpm) (29). The last aspect of the fetal heart rate tracing analyzed on an NST is heart rate variability, or the fluctuations in the fetal heart rate seen outside of accelerations or decelerations (29). Any deceleration lasting longer than 10 minutes is considered a change in baseline if the new rate is greater than 110 bpm, or bradycardia if the new heart rate is less than 110 bpm. Repetitive prolonged decelerations are cause for concern for fetal compromise. 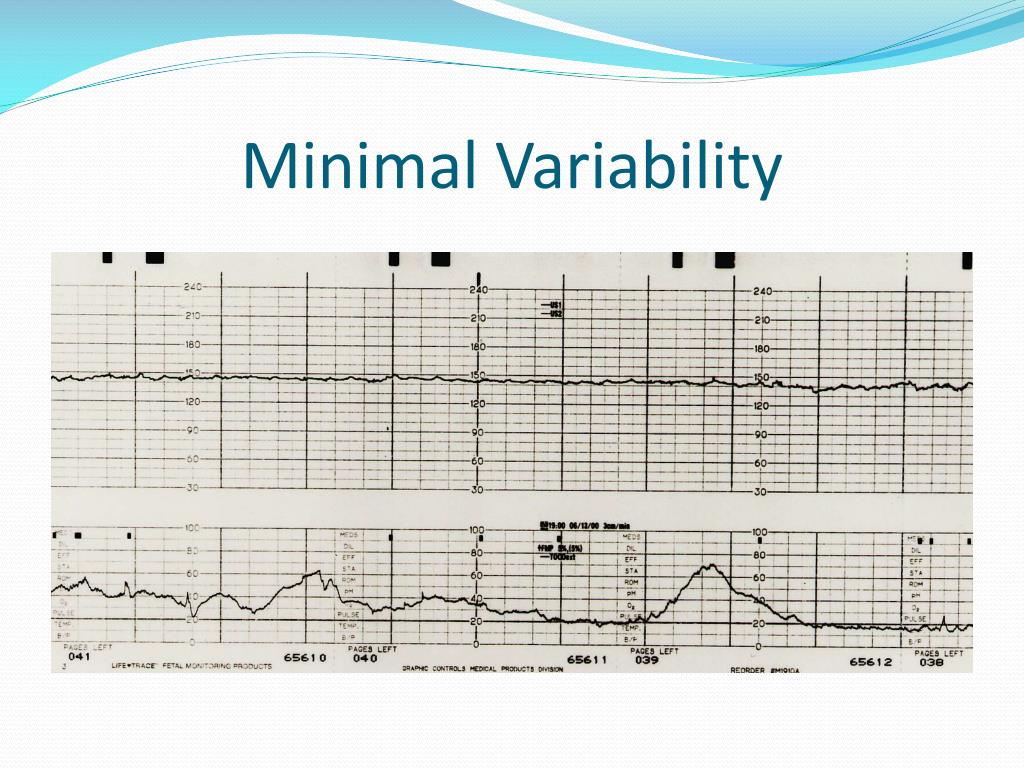
Prolonged decelerations: A prolonged deceleration is any deceleration at least 15 bpm below the baseline that lasts for 2 to 10 minutes (29).Persistence of late decelerations, especially in the absence of baseline fetal heart rate variability, is an ominous sign of fetal compromise. These decelerations occur as a result of decreased uteroplacental oxygen delivery to the fetus, but they may not necessarily signify poor placental function-late decelerations may be caused by maternal hypotension or decreased uterine blood flow. Their onset begins after the contraction begins, and they resolve after the resolution of the contraction (29) ( Fig. Late decelerations: Late decelerations occur late in relation to the uterine contraction.Repetitive moderate or severe variable decelerations may indicate fetal compromise. Mild or isolated variable decelerations are benign. “Shoulders” can be seen both preceding and following these variable decelerations, and should not be considered accelerations, as they are a manifestation of the increase in sympathetic nervous system stimulation during fetal heart rate decelerations. They are thought to be caused by intermittent umbilical cord compression. Variable decelerations do not necessarily correlate with contractions ( Fig. Variable decelerations: Variable decelerations are abrupt decreases in the fetal heart rate at least 15 bpm below baseline with the onset to nadir lasting less than 30 seconds.Early decelerations are thought to be benign and generally are not associated with fetal hypoxia, acidosis, or low Apgar scores. This pressure results in an alteration in cerebral blood flow and stimulation of the vagal center, causing parasympathetic stimulation and a subsequent decrease in the fetal heart rate. They are believed to be caused by pressure on the fetal head. Early decelerations: Early decelerations begin at the onset of uterine contractions and appear to mirror the contraction ( Fig.Therefore, each type of deceleration has different implications for fetal status. Different types of decelerations are caused by different mechanisms. Decelerations occur when the fetal heart rate falls below the baseline heart rate they are classified according to their appearance and location in relation to uterine contractions. CK, CK-MB, and left-to-right/bidirectional shunts at PFO and PDA were higher overall at 72 hours of age.Ĭonclusions: Category II FHR is associated with resuscitation at birth, NICU admission, and length of hospitalization.Fetal heart rate decelerations can also be appreciated on an NST or during continuous fetal monitoring during labor. 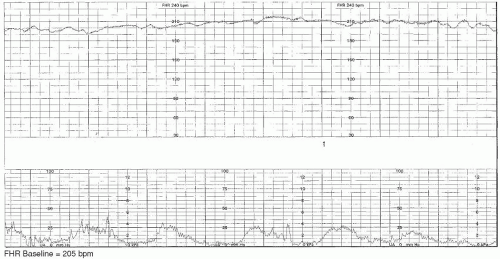
Indices of right (tricuspid annular plane systolic excursion : 7.3 ± 0.9 mm) and left ventricular performance (fractional shortening: 31% ± 8.9%, transmitral E’/A’ 0.9 ± 0.3) were low compared to normative data for healthy infants. 
Category II FHR pattern was associated with low pH at birth, and the need for resuscitation was more frequent among infants in the lower pH group (73% vs. Results: 23% (43/185) of infants of women detected with Category II FHR pattern needed NICU admission. The cohort was also stratified into three categories according to admission to NICU and pH threshold ( umbilical artery blood pH 7.15 and admitted not admitted). The primary outcome included the need for resuscitation and Neonatal Intensive Care Unit (NICU) admission. Category II trace was defined by the presence of tachycardia or bradycardia, variable and late decelerations, marked variability at least 30 minutes in the 120 minutes prior to delivery. Methods: A prospective study of 185 low-risk pregnant women in labor at > 37 0/7 weeks of gestation with a singleton fetus was conducted at a single center. Our aim was to compare low versus high pH cord blood infants of women detected with a Category II FHR pattern for which the impact is unclear. Background: The relationship between non-reassuring fetal heart rate (FHR) pattern, acidemia at birth and neonatal morbidity remains unclear. 
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
